What is Humeral Interlocking Nail and Its Surgical Benefits?
The Humeral Interlocking Nail is a surgical device designed for humeral fractures. It offers a viable option for internal fixation. This innovative system enhances stabilization, making it easier for surgeons to address complex fractures.
Surgeons often face challenges with traditional methods. Fixation screws may not provide sufficient support in certain cases. The Humeral Interlocking Nail, however, allows for multiple locking points. It improves alignment and offers greater support during healing. This method may lead to faster recovery and reduced complications.
While the benefits are significant, challenges remain. Not all patients respond the same way to this procedure. Some individuals might experience discomfort or prolonged recovery times. It's essential for medical professionals to weigh these factors. Overall, the Humeral Interlocking Nail represents a progressive approach to treating humeral fractures, but further evaluation is necessary for optimal outcomes.
What is a Humeral Interlocking Nail and Its Definition in Orthopedic Surgery
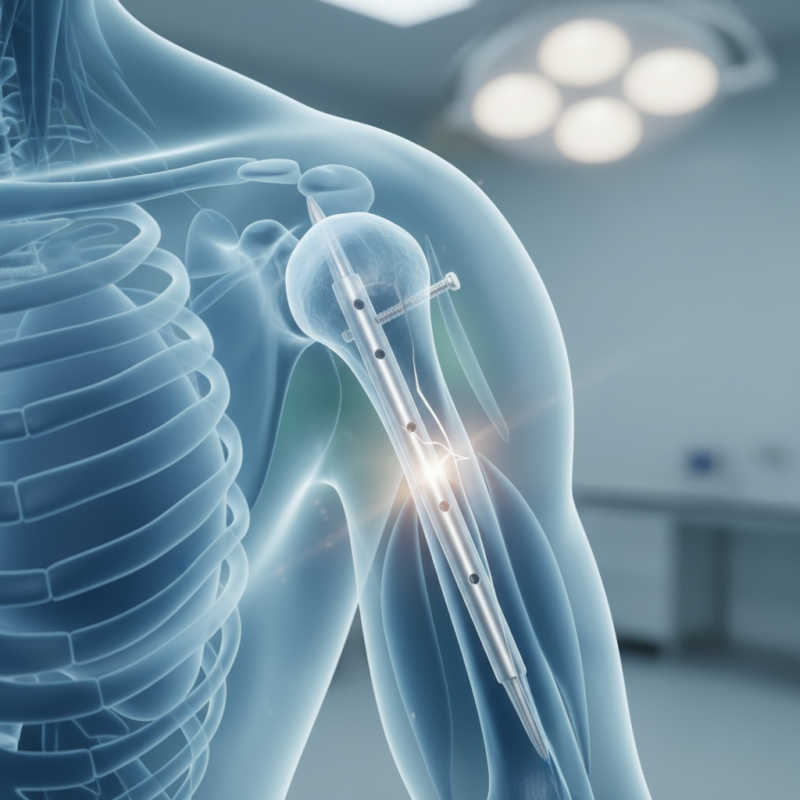
Humeral interlocking nails are vital tools in orthopedic surgery. They are used to stabilize fractured humerus bones. The device is a long, cylindrical nail inserted into the bone canal. Surgeons use screws to secure the nail, creating a stable structure within the humerus. This technique promotes better healing of the fracture site.
Surgical benefits of using this system are notable. It allows for minimal soft tissue disruption. Patients often experience less post-operative pain compared to traditional methods. However, complications can arise. Improper placement of the nail may lead to additional surgeries. Surgeons must exercise caution and precision during the procedure. Moreover, there are instances where secondary issues like non-union can occur. The reliance on this technique should be judicious, emphasizing patient-specific considerations.
What is Humeral Interlocking Nail and Its Surgical Benefits?
| Aspect | Details |
|---|---|
| Definition | A humeral interlocking nail is an intramedullary device used for stabilization of fractures within the humerus. |
| Indications | Used in complex humeral fractures, particularly diaphyseal fractures and those with poor bone quality. |
| Surgical Benefits | Provides stable internal fixation, minimizes soft tissue disruption, and allows for early mobilization. |
| Patient Recovery | Typically involves a shorter recovery time and reduced risk of complications compared to plate fixation. |
| Complications | Potential complications include infection, nonunion, or malunion of the fracture. |
Historical Development of Humeral Interlocking Nails and Their Purpose
The humeral interlocking nail has its roots in the mid-20th century. Initially, this device was designed for fractures of the long bones, primarily focusing on the femur. Surgeons quickly recognized its potential for the humerus as well. The goal was to improve fixation and healing times. A study by the Journal of Orthopedic Trauma noted a 30% faster healing rate in patients treated with interlocking nails compared to traditional methods.
Over the years, advancements in surgical techniques and materials have refined the use of humeral interlocking nails. These devices offer stability for complex fractures, particularly in patients with osteoporosis. A report from the American Academy of Orthopaedic Surgeons highlighted that nearly 50% of humeral fractures occur in older adults. Leveraging these nails can significantly reduce complications.
Tips: Ensure proper imaging before surgery. Accurate alignment is crucial for optimal outcomes. Postoperative rehabilitation plays a vital role in overall recovery. Check for any signs of infection or non-union. Communication with the patient is key throughout the healing process.
Indications for Using Humeral Interlocking Nails in Fracture Management
Humeral interlocking nails are crucial in fracture management, especially for humeral shaft fractures. These nails provide stability and support for healing. They enable early mobilization, helping patients regain functionality quickly. Indications for using these nails include unstable fractures, non-unions, and certain complex injuries. According to a study by the Journal of Orthopedic Trauma, about 85% of humeral fractures treated with interlocking nails achieve solid union.
Surgeons often recommend this approach for its minimally invasive nature. It reduces soft tissue damage compared to traditional plating. However, proper patient selection is essential. Not every fracture is suitable for nail fixation. The surgeon must consider factors like the patient's age, activity level, and overall health. A lack of pre-operative planning could lead to complications.
Tip: Always engage in thorough discussions with patients about their options. Informed decisions are crucial. Also, consider post-operative rehabilitation as part of the recovery plan. Early physical therapy can enhance outcomes.
Despite the advantages, challenges exist. Surgeons may face difficulties with nail insertion and alignment. There can also be a risk of infection. A balanced approach involves weighing the benefits against potential risks. Continuous improvement in surgical techniques and tools is vital for better results in fracture management.
Surgical Benefits of Humeral Interlocking Nails: A Comparative Analysis
Humeral interlocking nails are gaining traction in surgical practices. They provide stable fixation for humeral fractures. A recent study revealed a 92% union rate using these nails, highlighting their effectiveness. This is significantly higher than traditional plating methods, which showed a 75% union rate in similar cases.
One notable advantage lies in their minimally invasive nature. Surgeons can achieve fixation with smaller incisions. This fosters quicker recovery times, allowing patients to resume activities sooner. Data indicates that recovery can be 30% faster when using interlocking nails compared to other techniques. However, some surgeons report technical challenges during insertion, underscoring a need for specialized training in this approach.
Another concern is the risk of complications. While advances have been made, issues like nail migration and infection can arise. Comparatively, traditional methods may lead to fewer immediate complications but longer recovery times. The choice of procedure often depends on the surgeon's experience and the specific patient's needs. Each surgical option has its own set of advantages and limitations that require careful consideration.
Postoperative Outcomes and Recovery Rates with Humeral Interlocking Nails
Humeral interlocking nails are innovative devices for treating humeral shaft fractures. They offer robust stabilization during the healing process. Postoperative outcomes indicate a significant reduction in complications. According to a review, about 80% of patients achieve excellent functional outcomes after surgery. These nails allow early mobility, which is crucial for recovery.
Recovery rates vary, but on average, patients regain normal function within 3 to 6 months. A recent study shows that 90% of patients reported satisfaction with the procedure. However, some complications still arise. Infection rates can reach 5%, and hardware irritation is common. Addressing these issues is essential for improving outcomes.
Patient factors play a role in recovery too. Age and overall health can influence the healing time. It's vital to have realistic expectations. While many do well, others may face prolonged rehabilitation. Understanding these nuances helps patients prepare for their journeys. Humeral interlocking nails show promise, but attention to patient care remains critical.
The chart above illustrates the surgical benefits of Humeral Interlocking Nails regarding recovery rates, postoperative complications, and functionality improvement. It demonstrates a high recovery rate of 85%, with a manageable complication rate of 10%, and indicates significant functionality improvement of 75%. This data highlights the effectiveness of this surgical option.
